HIV and AIDS
“Oral tissues may reflect immune deficiency… nearly all HIV-infected individuals develop oral lesions at some time during their illness.” – U.S. Surgeon General’s Report
- What are HIV and AIDS?
- What other conditions can lead to immune deficiency?
- Should I tell my dentist if I have any of these conditions?
- What are the oral symptoms associated with HIV or AIDS?
- Will an HIV positive patient need special dental care or treatment?
- Can a dentist refuse to treat a patient with HIV or AIDS?
- How can the dentist and dental patients be protected from HIV and AIDS?
1. What are HIV and AIDS?
- The letters HIV stand for Human Immunodeficiency Virus.
HIV progressively destroys the body’s immune system.
- This virus eventually leads to AIDS.
The letters stand for Acquired Immunodeficiency Syndrome.
AIDS patients have a lowered natural immunity to infection, and so are prone to fatal illnesses.
Return to Questions
2. What other conditions can lead to immune deficiency?
- Chemotherapy and other conditions can cause an immune deficiency:
- Lupus
- Organ transplantation
- Leukaemia
- Tuberculosis
- Patients who have a damaged or deficient immune system are sometimes described as being immuno-compromised.
Return to Questions
3. Should I tell my dentist if I have any of these conditions?
- Yes, you should.
- Examination of your mouth will not necessarily show symptoms of these conditions.
- Your treatment may need to be modified if you have an immune system deficiency, so your dentist must be told.
Return to Questions
4. What are the oral symptoms associated with HIV or AIDS?
- The mouth can serve as an early warning that HIV has entered the system. Here is what may be evident:
- Candidiasis, also called thrush, is a fungal infection found with HIV.
- It is often an early warning symptom of HIV.
- It is usually found in people whose general health is poor.
- White patches appear on the palate and cheeks. They can be rubbed off leaving raw, red inflamed areas.
- It is treated with drugs or with topical medications.
- Toothbrushes should be discarded after each use, to assist the treatment.
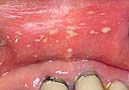
Thrush |
- Periodontitis and gingivitis is common with HIV, despite a careful programme of regular dental care.
- Antibiotics may be used to control the infection.
See Section on Periodontal Disease
- Hairy Leukoplakia is common with AIDS.
- It is sometimes the first symptom of HIV, and may indicate rapid progression to AIDS.
- Corrugated white lesions appear along the sides of the tongue.
- The lesions themselves have no other symptoms, and they do not respond to treatment.
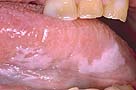
Leucoplakia |
- Xerostomia
- This is a persistently dry mouth and may accompany AIDS.
- It is not the ordinary dry mouth that can be cured by a glass of water.
- It can be caused by medication, mouth breathing, ageing, and an inadequate flow of saliva.
- Saliva substitutes in the form of mouthwashes, lozenges and toothpastes relieve the dryness.
- Sugarless chewing gum stimulates the flow of saliva and alleviates the dryness.
- Sialagogues stimulate saliva production and may be considered. Ask your doctor.
See Xerostomia
- Herpes Simplex
- This causes oral herpes, which is present in 50-60% of HIV patients.
- This is a chronic infection, with widespread painful blisters and ulcers.
- It is incurable. Medications may allow it to disappear for a time, but it will re-appear.
- It is spread by intimate physical contact.
- Infants can acquire it from their mothers during pregnancy or birth.
- In people with immune deficiencies it is particularly severe.
- Prolonged treatment may then be needed.
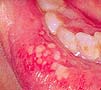
Herpes |
|
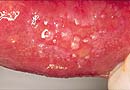
Herpes |
- Aphthous ulcers or canker sores
- These rounded painful shallow ulcers recur at intervals of a few days to a few months
- The ulcers are less than 5 mm. in diameter.
- They have a grey/white centre, with a red inflamed border.
- The lips, cheeks and the floor of the mouth are affected.
- The healing period is about 10-14 days.
- Chlorohexidine mouthrinses appear to have a beneficial effect.
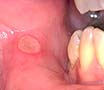
Canker sore |
- Squamous cell carcinoma and lymphoma
- This is the most common form of mouth cancer in the general population.
- It also occurs with HIV and AIDS.
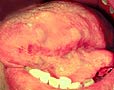
Cancer of the tongue |
|
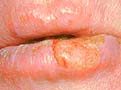
Cancer of the lip |
- Kaposi’s Sarcoma
- This is the most common form of cancer with HIV and AIDS.
- It is much more common in men than in women.
- Around a quarter of males with AIDS have this condition.
- It occurs on the skin as well as in the mouth.
- It is recognised as a purple to red swelling or as larger multiple nodular growths.
- Kaposi’s sarcoma is treated with a combination of surgery, radiotherapy, chemotherapy and biological therapy.
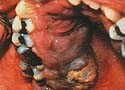
Kaposi’s sarcoma |
Return to Questions
5. Will an HIV positive patient need special dental care or treatment?
- People with HIV and AIDS are very prone to infection.
- Dental treatments should be preceded and followed by a chlorohexedrine mouthwash.
- There is no problem in carrying out routine dental treatments on immuno-compromised patients.
- Extractions will be covered by antibiotics and antimicrobial mouthwashes, at the appropriate times.
- HIV and AIDS patients may become allergic to antibiotics.
- A careful programme of professional cleaning and home dental care must be followed, to keep gingivitis and periodontitis under control.
Even if there are no symptoms to be seen, this strict pattern of oral hygiene should be followed:
- Twice daily brushing with a toothpaste containing fluoride, and flossing are essential.
- An antiseptic mouthwash containing fluoride will also aid plaque control.
Return to Questions
6. Can a dentist refuse to treat a patient with HIV or AIDS?
- Dentists have a moral, ethical and legal obligation to carry out all necessary treatment for all patients.
They do also have the right to decide whom they will treat.
This is a grey area in professional ethics.
Return to Questions
7. How can the dentist and dental patients be protected from HIV and AIDS?
- Certain precautions are now carried out routinely in all dental practices.
- Confirm with your own dentist that these precautions are carried out.
- The dentist and all assistants wear gloves and masks.
- The dentist and dental staff should be immunised against Hepatitis B. There is no immunisation against HIV and AIDS.
- All instruments are thoroughly cleaned, and sterilised by autoclave before re-use. Some instruments are not able to be autoclaved, but all possible precautions will be taken.
- Wherever possible, disposable equipment is used.(e.g. injection needles).
- All contaminated materials and needles are removed by a clinical waste disposal contractor.
Return to Questions
Copyright © 2012 of Simplyteeth – All rights reserved.
The material contained in Simplyteeth.com is offered as information only, see our full legal disclaimer.
This website has been invisibly watermarked to protect the copyright.
Site Map







